Mindfulness, often described as a state of being fully present and aware of one’s thoughts, feelings, and sensations, has gained […]
How to Foster Healthy Relationships
A healthy relationship is built on mutual respect, trust, and open communication. It requires effort, understanding, and a willingness to […]
The Role of Nutrition in Overall Health
Nutrition plays a crucial role in maintaining our overall health and well-being. The food we consume has a direct impact […]
The Connection Between Sleep and Mental Health
Sleep is a fundamental biological process that is crucial for our overall health and well-being. It plays a vital role […]
Tips for Avoiding Respiratory Infections
Respiratory infections can be quite common, especially during flu seasons or when you come into contact with someone who is […]
The Importance of Regular Health Check-ups
Regular health check-ups are an essential aspect of maintaining overall well-being and preventing potential health issues. These check-ups involve visiting […]
Protecting Your Bones: Osteoporosis Prevention
Osteoporosis is a condition that weakens your bones and makes them more susceptible to fractures and breaks. It affects millions […]
Achieving and Maintaining a Healthy Weight
Obesity and weight-related issues have become a global concern in recent years. Maintaining a healthy weight is not only important […]
Anxiety Management Techniques You Can Try Today
Anxiety is a common mental health condition that affects millions of people worldwide. It can manifest in various ways, such […]
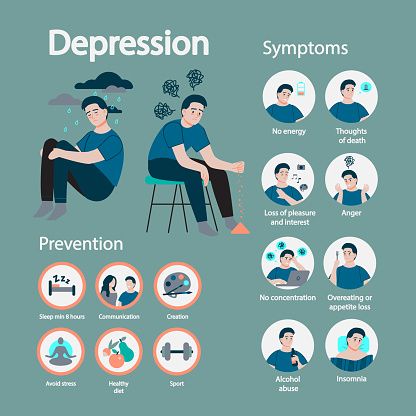
Depression: Signs, Symptoms, and Coping Strategies
Depression is a mental health disorder that affects millions of people worldwide. It can have a significant impact on an […]